Simple light dosimetry during endoscopic PDT treatments using an optical fiber with microlens.
- Biomedical Optics NewsETC., August 1, 1998, Steven L. Jacques, Oregon Medical Laser Center, Portland, OR
This article presents a simple dosimetry technique for setting the laser power during a photodynamic therapy (PDT) treatment that uses an optical fiber with a microlens which is delivered through an endoscope.
My colleague Dr. Greg Blair, Providence St. Vincent Medical Center, was planning a PDT treatment of laryngeal carcinoma using a protocol published by Dr. Merrill Biel (Northwestern Hospital Laser Center, Minneapolis): Photodynamic therapy and treatment of neoplastic diseases of the larynx. Laryngoscope 104:399-403, 1994. The procedure was approved by the hospital Internal Review Board (IRB).
- The photosensitizer was Photofrin (Sanofi).
- Irradiation of the larynx used an optical fiber with a microlens termination which concentrated the light into a more collimated and uniform forward-directed beam.
- The desired exposure was 0.150 W/cm2 at 630 nm for 533 min to yield 80 J/cm2.
At what power should the doctor set the laser during treatment?
The spot size of laser light on the target tissue depends on the fiber-target distance. So in the clinic, the doctor must adjust the laser power for a particular fiber-target distance to yield the desired irradiance of 0.150 W/cm2. The doctor can observe the delivery of the optical fiber to the larynx through the working channel of an endoscope, and can see the light from the aiming beam transmitted through the fiber (usually either white light or a red HeNe laser beam). We devised the following technique for choosing the laser power setting:
Step 1
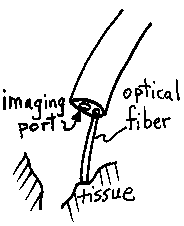
While the doctor controls the endoscope, the doctor verbally guides the nurse in feeding optical fiber through the working channel of the endoscope until the tip of the fiber is touching the target tissue. The fiber placement is observed through the endoscope through the viewing port, either by eye or using a video camera.
Step 2

The nurse marks the optical fiber with a marker pen where it exits the fiber channel of the endoscope outside the body.
Step 3

The doctor verbally guides the nurse in retracting the fiber causing the beam spot on the target tissue to expand until the spot size reaches the desired diameter that covers the intended treatment area.
Step 4

The spot of light on the target tissue due to the aiming beam of the laser system can be seen through the endoscope, either by eye or using a video camera.
h is the fiber-target distance.
Step 5

The nurse again marks the fiber where it exits the endoscope channel.
Step 6

The nurse measures the distance between the two marks on the fiber outside the body. This distance is the fiber-target distance h (cm).
Step 7
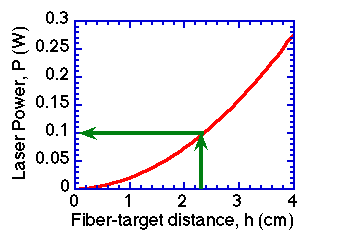
The laser operator finds the distance h on the x-axis of the CALIBRATION GRAPH, moves up on the graph to the curve, and moves over to the left y-axis to find the appropriate laser power setting in Watts.
Click here to learn how the calibration was accomplished. Our calibration is appropriate only for the particular microlens fiber that we purchased. A new calibration should be conducted for a microlens fiber with different model number or manufacturer.
Click here for enlarged version of calibration graph
Step 8
The laser operator sets the laser. The team starts the 533-s irradiation period.
The video camera view through the imaging bundle in the imaging port of the endoscope is blinded by the treatment laser, so the doctor cannot observe the treatment. Therefore, every two minutes a pause in the laser irradiation is made to allow the doctor to observe via the video camera and verify that the fiber placement has not inadvertantly moved. If the doctor observes by direct viewing while using laser safety glasses which block most of the treatment light, the doctor can observe the treatment real time.
We found the above protocol to be quite workable in the surgical suite environment. Dr. Blair also used the protocol during PDT without an endoscope while directly viewing the larynx down the throat. The protocol should be useful for dosimetry in general using microlens optical fibers with an endoscope. The basic idea would also be helpful when using a bare fiber.
The protocol is simple but provides only a first-order approximation to the desired light dosage. The angle, curvature, and roughness of tissue surfaces will complicate the light dosimetry somewhat. For example, if the tissue surface is slanting at 45 degrees, the power of a broad beam should be increased 40% above the power required for a tissue surface orthogonal to the beam, in order to account for how the beam spreads out over the slanted surface. If the beam is small (perhaps less than 5 mm diameter) there is significant lateral diffusion of light and the protocol underestimates the required laser power. But despite such subtleties in light dosimetery, the above protocol should approximately guide the laser power setting for a microlens fiber irradiating spots larger than 5 mm in diameter.
August NewsEtc |
PDT home page |
NewsETC. Contents page






